Your Eyes
- Home
- Your Eyes
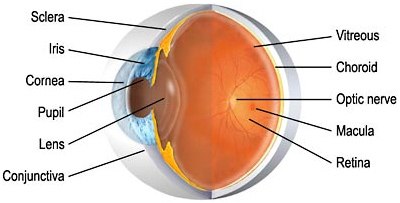
Normal Eye Anatomy
- The cornea is the clear, transparent front layer of the eye through which light passes.
- The iris gives our eyes color and it functions like the aperture on a camera, enlarging in dim light and contracting in bright light. The aperture itself is known as the pupil.
- The lens helps to focus light on the retina.
- The retina is the innermost layer of the back of the eye. This layer of light-sensitive nerve endings carries the visual impulse to the optic nerve. The macula is the central zone of the retina which provides our most central, acute vision.
- The optic nerve conducts visual impulses to the brain from the retina.
General Eye Examination
General eye examination is more than just getting your eyes checked for a lens prescription. It involves several tests to check your eyes for vision and for any eye disease.
The first comprehensive eye examination of the child should be done at 3 years unless some eye problem is noticed before that. Your ophthalmologist will check for normal 20/20 vision, lazy eye and crossed eye. If any vision problem is found the next regular eye checkup should be done as advised by your doctor. If not, the next eye checkup for the child should be done every two years. Early detection of any eye problem will help to provide timely treatment and thus will prevent deterioration of vision.
The first comprehensive eye examination of the child should be done at 3 years unless some eye problem is noticed before that. Your ophthalmologist will check for normal 20/20 vision, lazy eye and crossed eye. If any vision problem is found the next regular eye checkup should be done as advised by your doctor. If not, the next eye checkup for the child should be done every two years. Early detection of any eye problem will help to provide timely treatment and thus will prevent deterioration of vision.
Adults with normal vision in the age group of
- 20 to 40 years should go for general eye examination every 5 years.
- 40 to 65 years should go for it every 2 years.
- Above 65 years should go for it every year.
In case you have a family history of eye disease or vision problem or chronic disease such as diabetes that may affect vision, more frequent eye checkups would be required.
When you go for your eye examination the doctor will ask you about any vision problems you are facing or have had before and also about family history of diabetes, high blood pressure or heart disease. You should take your eyeglasses or contact lenses if using them along with you when going for the general eye examination.
General eye examination includes a number of tests that ascertain the health, function and appearance of different parts of the eye. They are:
When you go for your eye examination the doctor will ask you about any vision problems you are facing or have had before and also about family history of diabetes, high blood pressure or heart disease. You should take your eyeglasses or contact lenses if using them along with you when going for the general eye examination.
General eye examination includes a number of tests that ascertain the health, function and appearance of different parts of the eye. They are:
- Visual acuity test checks how well you can see from a distance of about 20 feet. You are asked to read aloud the letters written on a chart or screen (Snellen chart). The letters decrease in size as you read from the top line to the bottom line.
- Eye muscle test checks the function of the eye muscle used for movement of the eye. The doctor checks it by asking you to look at the pen or any other object without moving the neck when the doctor moves it in certain directions.
- Refraction test determines whether you need corrective lenses or your vision is normal. In case you need corrective lenses, it determines the prescription of lens that will give you the best possible vision. Your doctor may use computerized refractor or retinoscopy to determine your prescription for corrective lenses. In retinoscopy doctor shines a light into the eye after dilation and estimates the refractive error. Then fine adjustment for the prescription is done by making you decide which of the lenses when used in a mask like device -Phoroptor gives you the sharpest vision.
- Visual field test measures the peripheral or your side vision. It may be done using automated perimetry in which you will be asked to see into a special instrument that flashes light. If you see the light you have to press the button. It may also be determined by confrontation visual field exam in which you cover one of your eye and look at your doctor’s hand as it moves inward and outward from your visual field. You should tell your doctor when you are able to see his hand or fingers.
- Color Vision Test: In this test, the doctor will show you certain multicolored dot patterns. In case you have a certain color deficiency you will not be able to see certain patterns in those given sheets.
- Slit Lamp Examination: You are asked to sit and rest your chin and touch your forehead on the slit lamp. It magnifies the image of the eye and allows the doctor to look for any problem of the cornea, lens, iris and anterior chamber of the eye. Sometimes the doctor may stain the tear film of the eye with a fluorescein dye by using eye drop containing it or by using paper strip before examining through the slit lamp to look for cuts, foreign objects or infections of the cornea.
- Retinal examination is done to check for disease of the retina or optic nerve present at the back of the eye. The doctor will try to see the back of the eye using an ophthalmoscope or slit lamp following dilation of the pupil. The doctor may also choose to do indirect examination by using a bright light mounted on the head while each eye is kept open during examination. The eye drops used for examination will cause blurred vision and sensitivity to light for several hours even after the test. The effect will go away after a day or so.
- Glaucoma test is used to measure the internal eye pressure. It can be measured by :
Noncontact Tonometry: Here the blow of air on the eye is used to measure the eye pressure.
Applanation Tonometry: First your eye is numbed using eye drops. The eye drop also contains fluorescein to see the tear film. A gentle pressure is applied by touching the cornea using tonometer and eventually the amount of force required to flatten a part of the cornea temporarily is measured. The procedure does not hurt.
Pachymetry: After numbing the eyes an instrument is used to measure thickness of the cornea. It uses ultrasound waves to measure the same as corneal thickness is one of the significant factors that affect the intraocular pressure.
Your doctor will provide you the results of the tests within few days. In case any vision problem is detected the doctor will give you prescription for corrective glasses. However if any eye disease is detected or suspected you may be asked to go for specific eye test to confirm the initial finding.
Applanation Tonometry: First your eye is numbed using eye drops. The eye drop also contains fluorescein to see the tear film. A gentle pressure is applied by touching the cornea using tonometer and eventually the amount of force required to flatten a part of the cornea temporarily is measured. The procedure does not hurt.
Pachymetry: After numbing the eyes an instrument is used to measure thickness of the cornea. It uses ultrasound waves to measure the same as corneal thickness is one of the significant factors that affect the intraocular pressure.
Your doctor will provide you the results of the tests within few days. In case any vision problem is detected the doctor will give you prescription for corrective glasses. However if any eye disease is detected or suspected you may be asked to go for specific eye test to confirm the initial finding.
Types of Glaucoma
The different types of glaucoma include:
In this type of glaucoma, the angle between the iris and cornea is wide and open. As a result, the eye’s drainage system (trabecular meshwork) remains free of obstruction although increased resistance to fluid leaving the eye may still occur. This type of glaucoma may either be primary or secondary to other conditions such as pigment dispersion syndrome or pseudo exfoliation syndrome.
Primary open angle glaucoma (POAG) or chronic glaucoma is the most common type of glaucoma. As a chronic condition its effects occur slowly over time.
In Primary Open Angle Glaucoma, the drainage of the aqueous fluid from your eye doesn’t happen as well as it should and this causes the pressure to increase. Your eye may seem perfectly normal and your eyesight will seem to be unchanged – because when the pressure starts to build up it doesn’t cause you any pain – but your peripheral vision will still be getting damaged.
Your peripheral vision, which is the vision you have around the edge of what you are looking directly at, gradually gets worse. This type of glaucoma becomes more common over the age of 40, so you should have your eyes tested every two years.
In Primary Open Angle Glaucoma, the drainage of the aqueous fluid from your eye doesn’t happen as well as it should and this causes the pressure to increase. Your eye may seem perfectly normal and your eyesight will seem to be unchanged – because when the pressure starts to build up it doesn’t cause you any pain – but your peripheral vision will still be getting damaged.
Your peripheral vision, which is the vision you have around the edge of what you are looking directly at, gradually gets worse. This type of glaucoma becomes more common over the age of 40, so you should have your eyes tested every two years.
in this type of glaucoma, the angle between the iris and the cornea comes into contact resulting in a blocked trabecular meshwork. This may happen either quickly (acute) or slowly (chronic) and can be either primary or secondary to other conditions such as uveitis, neovascularization or iridocorneal endothelial syndrome (ICE).
This type of glaucoma occurs before the age of 2 years and often runs in families. It is caused by improper development of eye’s drainage channels before birth.
Diabetic Eye Disease – Retinopathy
Risk factors for Glaucoma:
- Age over 45 years
- Family history of glaucoma
- Black racial ancestry
- Diabetes
- History of elevated intraocular pressure
- Nearsightedness (high degree of myopia), which is the inability to see distant objects clearly
- History of injury to the eye
- Use of cortisone (steroids), either in the eye or systemically (orally or injected)
- Farsightedness (hyperopia), which is seeing distant objects better than close ones.
Diabetes is a chronic disease in which your blood glucose or sugar levels are very high. Uncontrolled levels pose a risk to associated heart, kidney, and eye disorders. People with diabetes may develop three major eye problems – glaucoma, cataract, and retinopathy. The early symptom of all these disorders is blurred vision. High blood sugar causes swelling of the lens in the eye, distorting the ability to focus clearly. Retinopathy is the most common eye disease associated with diabetes, and is one of the leading causes of blindness in adults.
Diabetic retinopathy is a disease which damages the tiny blood vessels in the retina (the light-sensitive tissue at the back of the eye). Having diabetes for a long time increases the chances of developing diabetic retinopathy.
Diabetic retinopathy is a disease which damages the tiny blood vessels in the retina (the light-sensitive tissue at the back of the eye). Having diabetes for a long time increases the chances of developing diabetic retinopathy.
There are three main types of retinopathy in diabetes, including:
Blood vessels are damaged, but vision is not affected.
The macula (center of the retina) is damaged. This significantly reduces your vision.
New blood vessels may grow from damaged blood vessels when the eye is deprived of oxygen. These new vessels are fragile and can bleed easily.
You chances of developing diabetic retinopathy increase with the following factors:
Causes and Complications:
- Long duration and poor control of diabetes
- High cholesterol
- High blood pressure
- Pregnancy
- Tobacco
High levels of sugar in your blood from diabetes can cause damage to the blood vessels supplying the retina and loss of sight when the vessels become blocked and blood supply is cut off. In response, the eye grows new vessels, but these do not develop properly, and can leak and cause vision loss. Scar tissue can also form, pulling the retina and causing it to detach.
Symptoms
The early stages of the disease do not show any symptoms; but as the condition worsens you may have blurred vision, spots or dark shapes floating in your vision (floaters), lowered night vision, or temporary or permanent blindness.
Diagnosis
Dilated eye exam is a good diagnostic tool for retinopathy. Drops will be placed in your eye to dilate your pupils (the black of your eye). This will help your doctor look for the presence of cataract, abnormal or new blood vessels, swelling, blood or fat deposits in the retina, scar tissue and retinal detachment.
Tests for vision and eye pressure will be performed.
Fluorescein angiography may be performed, in which a special dye is injected into your arm and images of the blood vessels are taken as the dye circulates into the eye. This will show the blood vessels that are broken, leaking or blocked.
Optical coherence tomography takes sectional images of the retina to determine leakage into the retinal tissue.
Diagnosis is critical, as if it is not detected and treated early, diabetic retinopathy can eventually lead to blindness.
The retina is a tissue present at the back of the eye that is responsible for vision. Severe near-sightedness, eye injury, cataract surgery or familial history may cause a retinal tear that can lead to retinal detachment. The retina is attached to the choroid tissue which provides the blood supply to the retina. When the retina tears, it gets detached from the choroid tissue along with its blood supply. A retinal tear is characterized by symptoms such as the appearance of floaters (small moving spots in the vision field), flashes of light in front of the eyes, darkening of your side vision and gradual loss of vision.
Detachment of the retina and retinal tears can be diagnosed by a complete and thorough check-up of your eye. Your doctor may gently apply pressure on your eye with a blunt instrument or cotton swab, and shine a bright light to examine the retina. Additional eye tests may be ordered, such as eye pressure test, vision test and ultrasound, to determine the cause of symptoms.
Detachment of the retina and retinal tears can be diagnosed by a complete and thorough check-up of your eye. Your doctor may gently apply pressure on your eye with a blunt instrument or cotton swab, and shine a bright light to examine the retina. Additional eye tests may be ordered, such as eye pressure test, vision test and ultrasound, to determine the cause of symptoms.
A cataract is a condition which causes clouding of the lens in the eye, resulting in blurry vision.
Human Lens
The lens is situated behind the iris, the dark portion of the eye, and is not visible. The lens is mostly made up of water and proteins. These specific proteins provide the lens its transparent structure. Any structural change in these proteins can alter the clarity of the lens and negatively impact vision. The lens becomes cloudy when a cataract occurs and is seen as a white cloudy ball in the center of the iris.
Classification of Cataract
Cataracts are classified based on their location in the eye. They include:
Nuclear Cataract: Cloudiness is present in the center of the lens.
Cortical Cataract: Cloudiness is seen in the outer peripheral or cortical region of the lens.
Subcapsular Cataract: Occurs at the back of the lens capsule or subcapsular region. This develops faster than the nuclear and cortical cataracts.
Causes
The development of a cataract is common in aged individuals due to related changes that occur in the structure of the lens proteins. Cataracts can also be inherited or can develop in infants as a result of infections in the mother during pregnancy. They can form as a complication of other diseases such as glaucoma and diabetes, or can develop after certain injuries. Prolonged use of corticosteroid inhalers and eye drops, and excessive exposure to UV rays, X-rays and other radiation during radiotherapy can increase the risk of cataract formation.
Diagnosis
To assess the impact of the cataract on your vision your doctor will perform a Visual Acuity Test where the patient reads an eye chart from a particular distance with one eye at a time. The doctor then examines the cornea, iris, and lens to detect any abnormalities.
Human Lens
The lens is situated behind the iris, the dark portion of the eye, and is not visible. The lens is mostly made up of water and proteins. These specific proteins provide the lens its transparent structure. Any structural change in these proteins can alter the clarity of the lens and negatively impact vision. The lens becomes cloudy when a cataract occurs and is seen as a white cloudy ball in the center of the iris.
Classification of Cataract
Cataracts are classified based on their location in the eye. They include:
Nuclear Cataract: Cloudiness is present in the center of the lens.
Cortical Cataract: Cloudiness is seen in the outer peripheral or cortical region of the lens.
Subcapsular Cataract: Occurs at the back of the lens capsule or subcapsular region. This develops faster than the nuclear and cortical cataracts.
Causes
The development of a cataract is common in aged individuals due to related changes that occur in the structure of the lens proteins. Cataracts can also be inherited or can develop in infants as a result of infections in the mother during pregnancy. They can form as a complication of other diseases such as glaucoma and diabetes, or can develop after certain injuries. Prolonged use of corticosteroid inhalers and eye drops, and excessive exposure to UV rays, X-rays and other radiation during radiotherapy can increase the risk of cataract formation.
Diagnosis
To assess the impact of the cataract on your vision your doctor will perform a Visual Acuity Test where the patient reads an eye chart from a particular distance with one eye at a time. The doctor then examines the cornea, iris, and lens to detect any abnormalities.
Unlike the normal curvature of the cornea, those suffering from this degenerative disorder have structural corneal changes leading to the appearance of a thin conical shaped cornea. This further affects the vision leading to distorted images, multiple images and sensitivity to light. Our ophthalmologist can help restore the vision by carrying out surgical procedures, namely crosslinking and customized wave front guided surface ablation. For advanced keratoconus, we also offer corneal ring segment inserts in order to flatten out the peak of the corneal cone.
Signs and Symptoms:
Initially, patients will experience blurring and distortion of vision, due to the progressive thinning of the cornea. This may be corrected with glasses during the early stages of the condition.
Signs and Symptoms:
Initially, patients will experience blurring and distortion of vision, due to the progressive thinning of the cornea. This may be corrected with glasses during the early stages of the condition.
The eye is a delicate and sensitive organ. An injury to the eye from contact sports or a motor vehicle accident can often result in trauma to the orbit. The orbit is the bony cavity of the skull that surrounds and protects the eye ball and includes muscles and nerves attached to the eye. The most common orbital injuries/disorders include orbital trauma and orbital tumors.
Orbital Trauma
Orbital trauma may be associated with bruising and fracture of the orbital bone. If the trauma is severe, quick action needs to be taken to minimize the risk of long-term damage or vision impairment. Orbital trauma can be broadly classified into two types:
Blunt Force Trauma: This type of trauma is more common in children. While at play, children may fall from a bicycle or engage in fist fights causing blunt force trauma which may break the bony orbit.
Penetrating and Perforating Trauma: This type of trauma is generally seen in adults and is one of the most severe forms of eye injuries. Motor vehicle accidents or accidents in the workplace involving sharp tools may cause irreparable damage to the eye.
Orbital traumas may lead to eye problems such as double vision, painful eye movement and dramatic alterations to the normal anatomy of the orbit leading to disfigurement. , In severe injury when the eye cannot be saved, reconstructive surgery is employed to place a prosthetic eye. Treatment options will depend on the particular injury sustained. The treatment goal is to restore function and preserve aesthetics of the face.
Orbital Trauma
Orbital trauma may be associated with bruising and fracture of the orbital bone. If the trauma is severe, quick action needs to be taken to minimize the risk of long-term damage or vision impairment. Orbital trauma can be broadly classified into two types:
Blunt Force Trauma: This type of trauma is more common in children. While at play, children may fall from a bicycle or engage in fist fights causing blunt force trauma which may break the bony orbit.
Penetrating and Perforating Trauma: This type of trauma is generally seen in adults and is one of the most severe forms of eye injuries. Motor vehicle accidents or accidents in the workplace involving sharp tools may cause irreparable damage to the eye.
Orbital traumas may lead to eye problems such as double vision, painful eye movement and dramatic alterations to the normal anatomy of the orbit leading to disfigurement. , In severe injury when the eye cannot be saved, reconstructive surgery is employed to place a prosthetic eye. Treatment options will depend on the particular injury sustained. The treatment goal is to restore function and preserve aesthetics of the face.
Orbital trauma may be associated with bruising and fracture of the orbital bone. If the trauma is severe, quick action needs to be taken to minimize the risk of long-term damage or vision impairment. Orbital trauma can be broadly classified into two types:
Blunt Force Trauma: This type of trauma is more common in children. While at play, children may fall from a bicycle or engage in fist fights causing blunt force trauma which may break the bony orbit.
Penetrating and Perforating Trauma: This type of trauma is generally seen in adults and is one of the most severe forms of eye injuries. Motor vehicle accidents or accidents in the workplace involving sharp tools may cause irreparable damage to the eye.
Orbital traumas may lead to eye problems such as double vision, painful eye movement and dramatic alterations to the normal anatomy of the orbit leading to disfigurement. , In severe injury when the eye cannot be saved, reconstructive surgery is employed to place a prosthetic eye. Treatment options will depend on the particular injury sustained. The treatment goal is to restore function and preserve aesthetics of the face.
Blunt Force Trauma: This type of trauma is more common in children. While at play, children may fall from a bicycle or engage in fist fights causing blunt force trauma which may break the bony orbit.
Penetrating and Perforating Trauma: This type of trauma is generally seen in adults and is one of the most severe forms of eye injuries. Motor vehicle accidents or accidents in the workplace involving sharp tools may cause irreparable damage to the eye.
Orbital traumas may lead to eye problems such as double vision, painful eye movement and dramatic alterations to the normal anatomy of the orbit leading to disfigurement. , In severe injury when the eye cannot be saved, reconstructive surgery is employed to place a prosthetic eye. Treatment options will depend on the particular injury sustained. The treatment goal is to restore function and preserve aesthetics of the face.
Those diagnosed with strabismus have mis-aligned eyes, due to lack of coordination between the extraocular muscles. This can lead to improper double vision. Our ophthalmologist here can help correct this with a combination of eyeglasses, vision therapy and surgery.
What is Strabismus?
Strabismus is used to describe the disorder where the eyes do not line up together in the same direction. Six different muscles surround the eyes and work together to ensure both eyes can focus on the same object. In someone with strabismus, these muscles do not work together. As a result, one eye looks at one object, while the other eye turns in a different direction and is focused on another object. The squinting eye can turn inwards (convergent), outwards (divergent), up or down. When squinting occurs, two different images are sent to the brain, one from each eye. This confuses the brain, and the brain may learn to ignore the image from the weaker eye. Someone with strabismus may also experience difficulty with depth perception.
Types of Squints:
The most common types of squint are as follows:
Infantile squint – This type of squint occurs within the first few months of life.
Accommodative squint – This occurs in children who are long sighted. The eyes can focus very hard to overcome the long sight, but as a result the eye over converges (turns in) and a squint develops. The age of onset for this type of squint varies from 2-6yrs.
Abnormal vision – If your child has reduced vision in one or both eyes a squint can develop.
Illness – Sometimes squints become obvious after a childhood illness e.g. chicken pox or measles. This is rarely the cause but the poor general health has reduced the ability to control the eyes and the result is a squint.
Strabismus can also be seen in adults when there is presence of other disorders such as, brain & nerve disorder, diabetes, injuries to eye and tumor in the eye or brain.
What are the implications of a squint?
Amblyopia (lazy eye) – If a child develops a squint he/she ‘switches off’ the eye that turns to avoid experiencing improper double vision. If left untreated the vision can deteriorate and result in amblyopia, also known as lazy eye.
What is Strabismus?
Strabismus is used to describe the disorder where the eyes do not line up together in the same direction. Six different muscles surround the eyes and work together to ensure both eyes can focus on the same object. In someone with strabismus, these muscles do not work together. As a result, one eye looks at one object, while the other eye turns in a different direction and is focused on another object. The squinting eye can turn inwards (convergent), outwards (divergent), up or down. When squinting occurs, two different images are sent to the brain, one from each eye. This confuses the brain, and the brain may learn to ignore the image from the weaker eye. Someone with strabismus may also experience difficulty with depth perception.
Types of Squints:
The most common types of squint are as follows:
Infantile squint – This type of squint occurs within the first few months of life.
Accommodative squint – This occurs in children who are long sighted. The eyes can focus very hard to overcome the long sight, but as a result the eye over converges (turns in) and a squint develops. The age of onset for this type of squint varies from 2-6yrs.
Abnormal vision – If your child has reduced vision in one or both eyes a squint can develop.
Illness – Sometimes squints become obvious after a childhood illness e.g. chicken pox or measles. This is rarely the cause but the poor general health has reduced the ability to control the eyes and the result is a squint.
Strabismus can also be seen in adults when there is presence of other disorders such as, brain & nerve disorder, diabetes, injuries to eye and tumor in the eye or brain.
What are the implications of a squint?
Amblyopia (lazy eye) – If a child develops a squint he/she ‘switches off’ the eye that turns to avoid experiencing improper double vision. If left untreated the vision can deteriorate and result in amblyopia, also known as lazy eye.
Ptosis is the medical term for a condition in which the upper eyelid droops down slightly or in severe cases, the lid droops low enough to cover the whole pupil and block normal vision. Ptosis can occur in both children and adults.
A number of factors may contribute to the development of ptosis. These include:
Weakening of the levator muscles (muscles of the upper eye lid) from ageing or may be present at birth
Brain and spinal cord injuries resulting in weakening of facial and eye muscles
Auto-immune diseases such as Myasthenia gravis
Cluster headaches
If you have ptosis, there would be a visible drooping of the upper eyelid, giving the eye a smaller than usual appearance. You may also unconsciously raise your eyebrows and tilt your head frequently to have a better view of objects.
Treatment methodology of ptosis in adults and children varies depending on the cause.
Imperial Healthcare is a center par excellence widely recognized for providing quality eye care to its patients. Imperial Healthcare’s core team comprises of a certified and well experienced ophthalmologist Dr. Vinod Gauba who has mastered the latest cutting edge technology advancements for managing a wide range of complex eye disorders.
A number of factors may contribute to the development of ptosis. These include:
Weakening of the levator muscles (muscles of the upper eye lid) from ageing or may be present at birth
Brain and spinal cord injuries resulting in weakening of facial and eye muscles
Auto-immune diseases such as Myasthenia gravis
Cluster headaches
If you have ptosis, there would be a visible drooping of the upper eyelid, giving the eye a smaller than usual appearance. You may also unconsciously raise your eyebrows and tilt your head frequently to have a better view of objects.
Treatment methodology of ptosis in adults and children varies depending on the cause.
Imperial Healthcare is a center par excellence widely recognized for providing quality eye care to its patients. Imperial Healthcare’s core team comprises of a certified and well experienced ophthalmologist Dr. Vinod Gauba who has mastered the latest cutting edge technology advancements for managing a wide range of complex eye disorders.
Eyelid retraction is a condition characterized by the upward displacement of the upper eyelid or downward displacement of the lower eyelid thereby exposing the sclera (white part of the eye). Lower eyelid retraction may be a result of shallow orbits (deepened bony eye sockets), hereditary conditions or certain characteristics of the eyelid.
Eyelid retraction can lead to a wider than normal opening of the eyelids producing a wide eyed stare and causing drying of the eyes. This condition may irritate the ocular structure, cause vision discomfort and harmful effects on the cornea.
Causes
The most common cause of lower eyelid retraction is thyroid eye disease (TED). TED leads to inflammation and fibrosis (excessively formed tissue) of the retractor muscles of the eyelid thereby causing retraction. Other causes include:
Too much tissue removal and damage to the lower eyelid during cosmetic repair of the lower eyelid (blepharoplasty)
Trauma to the eye
Eyelid retraction can lead to a wider than normal opening of the eyelids producing a wide eyed stare and causing drying of the eyes. This condition may irritate the ocular structure, cause vision discomfort and harmful effects on the cornea.
Causes
The most common cause of lower eyelid retraction is thyroid eye disease (TED). TED leads to inflammation and fibrosis (excessively formed tissue) of the retractor muscles of the eyelid thereby causing retraction. Other causes include:
Too much tissue removal and damage to the lower eyelid during cosmetic repair of the lower eyelid (blepharoplasty)
Trauma to the eye
This is a common condition and is caused by a blockage in one of the small glands in the eyelid. A small lump develops as the normal contents cannot escape. Although it is unsightly, it is easy to treat and should not cause you any major problems with your vision.
As a first step in treatment, you will be prescribed antibiotics to reduce the inflammation in the eyelid. Heat treatment with hot compresses can also help and may actually release the contents of the cyst which means that further intervention is not needed.
If it has not resolved on this treatment, it can be removed surgically. Your name will be put on the minor operations waiting list and you will be given a date to come in for the procedure.
Treatment
Center for Sight
The Eyelid Clinic
Skin & Hair
Acupuncture
SupraLIFT™
Our Doctors
Dr. Vinod Gauba
Dr. Qasim Aref Qasem
Dr. Radha Lachhiramani
Dr. Sanghee Won
Dr. Alaa Al-Dabbagh
Dr. Samer Hamada
Dr. Tina Eckert
Facility - Imperial Healthcare - InstituteFACILITIES
Recent Advancements - Imperial Healthcare - InstituteRECENT ADVANCEMENTS
Testimonials - Imperial Healthcare - InstitutePATIENTS’ EXPERIENCES
Dubai Healthcare City
As a first step in treatment, you will be prescribed antibiotics to reduce the inflammation in the eyelid. Heat treatment with hot compresses can also help and may actually release the contents of the cyst which means that further intervention is not needed.
If it has not resolved on this treatment, it can be removed surgically. Your name will be put on the minor operations waiting list and you will be given a date to come in for the procedure.
Treatment
Center for Sight
The Eyelid Clinic
Skin & Hair
Acupuncture
SupraLIFT™
Our Doctors
Dr. Vinod Gauba
Dr. Qasim Aref Qasem
Dr. Radha Lachhiramani
Dr. Sanghee Won
Dr. Alaa Al-Dabbagh
Dr. Samer Hamada
Dr. Tina Eckert
Facility - Imperial Healthcare - InstituteFACILITIES
Recent Advancements - Imperial Healthcare - InstituteRECENT ADVANCEMENTS
Testimonials - Imperial Healthcare - InstitutePATIENTS’ EXPERIENCES
Dubai Healthcare City
For Appointments
Please feel welcome to contact our friendly reception staff with any general or medical enquiry call us.
Opening Hours
Sat – Wed 10.00 AM – 7:00 PM
Thursday 10.00 AM – 2:00 PM
Friday Closed
